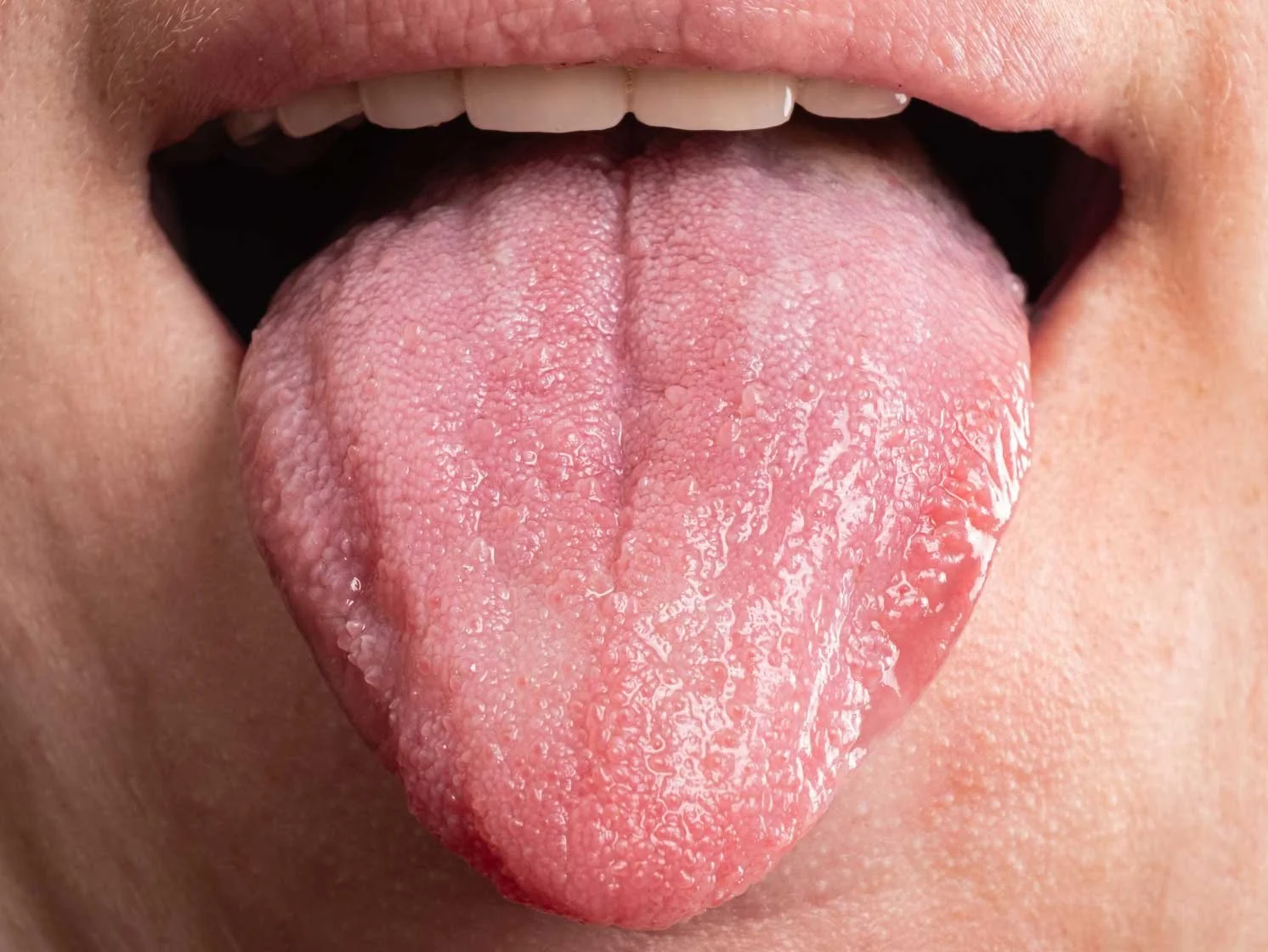
Oral Cancer's Tendency to be "Multifocal" – Meticulous Tracking is Vital!
The "five-year survival rate of cancer patients" is a significant metric for evaluating the success of a hospital's treatments, reflecting the survival status of patients five years after beginning treatment. However, to assess medical quality more objectively, additional factors must be considered, such as the type and stage of the patient's cancer, treatment methods, overall health status, socioeconomic standing, family situation, follow-up tracking and support, as well as the patient's quality of life. According to our hospital's cancer registry, the five-year observed survival rate for our oral cancer patients from 2015 to 2019 is 73%, which surpasses the national data. Overall, I attribute this success to the patients having robust family support combined with detailed and uninterrupted follow-up tracking.
Why is Oral Cancer Prone to be "Multifocal"?
Oral cancer is known to be "multifocal," meaning that cancer can occur multiple times in different locations. This is because the entire oral mucosa and even the pharynx, esophagus, and lungs of patients have been exposed long-term to carcinogens such as tobacco, alcohol, and areca nut. Therefore, pathological changes can occur in many areas, with symptoms appearing at different times. As long as the mucosa remains, there is the potential for new cancer development. This is why we often tell patients that the likelihood of multiple occurrences of oral cancer is higher compared to other types of cancer.
Family Support and Follow-Up Tracking
Meticulous and continuous follow-up work is a key factor in helping oral cancer patients to detect second, third, or fourth occurrences of cancer early and to deal with them promptly—this is crucial for extending the survival period of patients. However, how can we ensure uninterrupted patient follow-up? This relies on two main conditions. The first is the power of family support. From my observations, if a patient is accompanied by family or children to the hospital, and after surgery has someone to help care for wounds and nutrition, they generally can return for follow-up appointments on time. As a result, their recovery tends to be better, and their survival period longer. The second condition is a good doctor-patient relationship. Due to Taiwan's National Health Insurance system, it is very convenient to register and transfer to any hospital across Taiwan. It's normal for patients to lose faith in their original hospital and doctor when they get oral cancer again and want to switch to another hospital for treatment. But I advise patients to continue treatment and follow-up with a doctor they trust, to let the doctor who is most familiar with their condition diagnose and treat them. Because oral cancer is prone to recurrence, from the first diagnosis of oral cancer, over the next five or even ten years, the doctor needs to repeatedly check and perform minor surgeries. This is unlike other cancers where treatment is usually concentrated in the first six months or year. Typically, oral cancer patients need more frequent follow-ups during the first five years after treatment, and should still follow up one to two times a year after five years. Based on my observations, the recurrence rate of oral cancer in our institution is not lower, but many patients can detect and manage it in time. As long as oral cancer patients and doctors become good comrades-in-arms, the patient's survival period can be expected to extend.
Standing in the Patient's Shoes
Patients with head and neck cancer are less likely to undergo chemotherapy in addition to surgery and radiation because head and neck cancer is a type of squamous cell carcinoma, which has low sensitivity to chemotherapy. Targeted treatments that are highly effective for breast and lung cancer offer only limited benefits for patients with metastatic head and neck cancer. More than three years ago, when immunotherapy for head and neck cancer began to be covered by national health insurance, it indeed helped a portion of patients. However, due to the high costs of immunotherapy and the stringent conditions for health insurance coverage, not many patients can actually receive this benefit. Moreover, many head and neck cancer patients are blue-collar workers, and the proportion who can afford the costs on their own is also not high. When patients are faced with the choice of whether or not to use immunotherapy, our head and neck cancer medical team stands in the position of the patients and their families, providing them with objective clinical data and having detailed discussions with them before deciding together on the next treatment plan. We are acutely aware that the tone and manner in which a physician communicates with patients will profoundly influence the decisions the patients make next, and these decisions will bring significant changes to both the individual and their entire family. Therefore, we understand that our daily work is not just about treating a person's "disease," but rather about properly caring for a sick "person."
Author: Dr. Shyuang-Der Terng (Otolaryngology and Head & Neck Surgery)