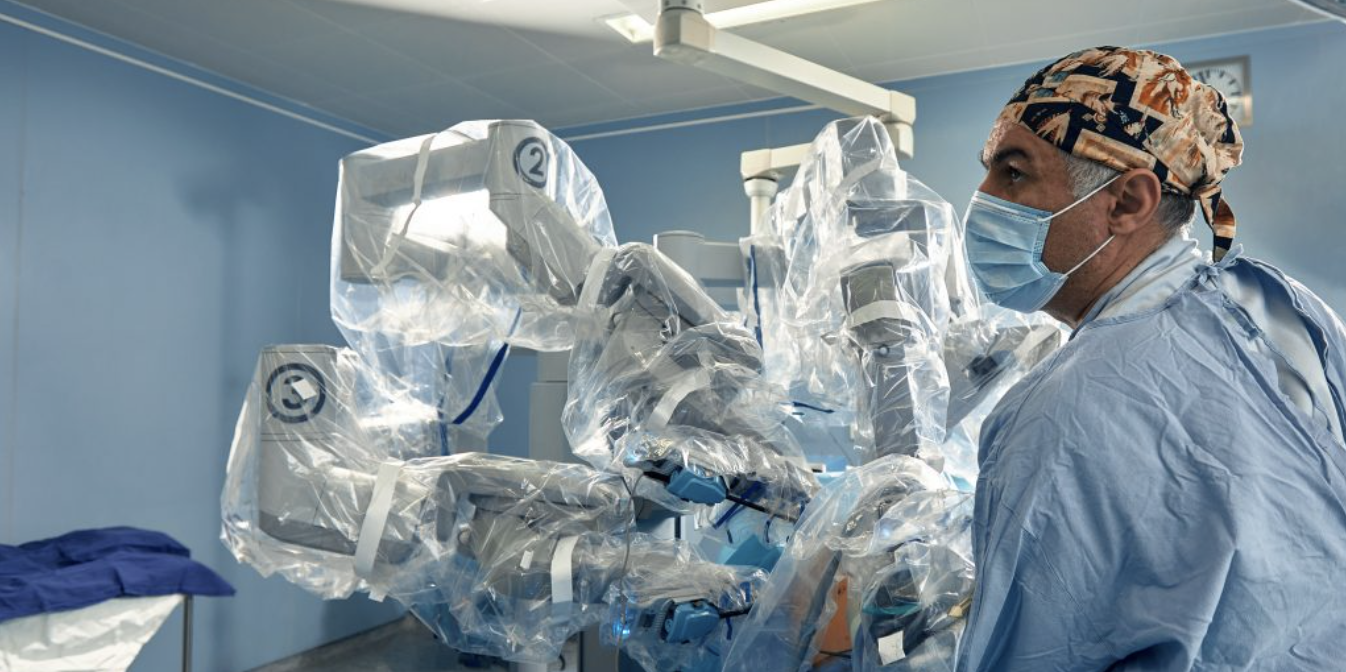
One Woman’s Choice Between the da Vinci Robot and the Surgeon’s Knife
by Pharmacist Fang Li-Hua
When her teenage daughter held up blood-stained laundry in January 2021, a 55-year-old post-menopausal accountant realized the bleeding she had brushed aside could no longer stay hidden. The two traveled from Taiwan’s east coast to the local hospital, where a diagnostic dilation-and-curettage uncovered the culprit: endometrioid adenocarcinoma, Stage IB—a tumor confined to the uterus yet already halfway into its muscle.
The attending physician praised the da Vinci robotic system: keyhole incisions, one-night hospitalization, a swift return to normal life. The price—about NT $300,000 out-of-pocket—was steep for a single-income family without private insurance, so mother and daughter headed to Taipei for a second opinion at Koo Foundation Sun Yat-Sen Cancer Center.
The hidden scar
At the clinic, she described nagging lower-abdominal pain that had persisted since childbirth and recently worsened, plus occasional soreness under both ribs. She had slept on her side for decades because lying flat felt like tugging on an unseen cord. MRI solved the puzzle: a 19 mm irregular lesion in the uterine fundus spared the deeper muscle, but the anterior uterine wall was welded to the abdominal wall, a legacy of a long-ago cesarean section.
Two roads, one decision
Dr. Wang Zong-De laid out the choices in plain language.
With the robot: Jointed wrists and magnified 3-D vision could tease apart those dense scars. The operation would begin with meticulous pelvic and para-aortic lymph-node removal, then the uterus would be detached using a uterine manipulator anchored inside the cavity for leverage. Critics worry that manipulating a cancer-filled organ—or accidentally breaching its wall in the gas-filled abdomen—might seed tumor cells across the peritoneum, though hard proof remains elusive.
With an open incision: Surgeons would first lift out the uterus and ovaries, then clear the lymph nodes. If the old scar tore the uterine wall, packs could isolate the cavity within seconds, limiting any spill. The trade-off was obvious: a larger scar, several days in the ward, a slower recovery.
Given the tight cesarean adhesions, even a flawless robotic approach would demand extensive dissection in cramped space, leaving little margin if the wall gave way. Dr. Wang’s creed—the first cancer operation shapes every tomorrow—guided the family to choose the larger cut and, they believed, the safer cure.
Why many still favor the robot
Pinpoint accuracy in narrow pelvic corners saves nerves and vessels.
Cleaner lymph-node harvest refines staging and adjuvant-therapy plans.
Less blood loss and lower infection rates speed discharge—vital for frail patients.
Faster bounce-back lets chemo- or radiotherapy start sooner.
Minimally invasive trauma can be the only workable option for the very elderly.
Why others decline
Hardware, disposables, and longer OR time drive up cost.
Surgeons see everything but feel nothing; tactile clues vanish at the console.
Advanced cases demand a steep learning curve and high case volume.
Bulky or widely metastatic tumors may outrun the system’s reach.
In very extensive disease, some studies show lower rates of truly clear margins than open surgery.
Dr. Wang summed it up for his residents: “Safety outranks elegance. Accept a hand-span of scar today, and every step after is on firmer ground.”